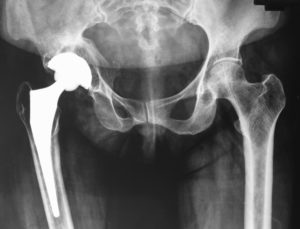
The hip is a ball-and-socket joint, which allows a wide range of movement. Arthritis damages the cartilage-covered surfaces of the joint so the ball moves less smoothly and less freely within the socket. Full function of the hip joint depends on the successful coordination of many interrelated parts, including bones, muscles, tendons, ligaments, and nerves. Even though the hip joint is exceptionally stable, it can be injured by overuse in sports, or due to aging disease and trauma. In a hip replacement or resurfacing operation, the surgeon replaces the damaged surfaces with artificial parts, which may be made of metal, plastic or ceramic materials.
WHO NEEDS A HIP REPLACEMENT?
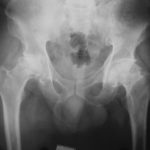
Hip replacement is most commonly recommended for severe osteoarthritis, but it’s sometimes used for inflammatory conditions such as rheumatoid arthritis or ankylosing spondylitis or for problems with development of the hip during childhood. Hip surgery may also be needed for fractures of the hip, including those resulting from osteoporosis. Your doctors will always try other measures before suggesting a hip replacement – for example, painkillers, physiotherapy and/or walking aids, or occasionally a steroid injection into your hip joint. Typically, a diagnostic X-Ray shows whether a hip replacement is required or not. The doctor will also assess your fitness for surgery based on several parameters.
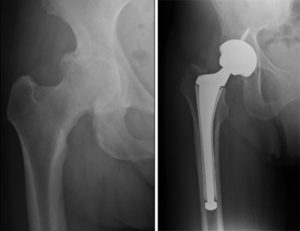
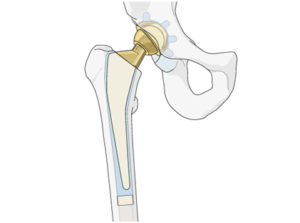
HIP JOINT SURGERIES
In addition to conservative management, we offer various surgical treatments which include:
TOTAL HIP REPLACEMENT (THR)
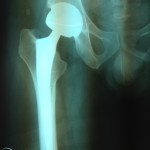
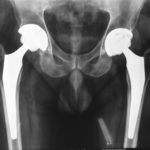
This is performed for painful conditions of the hip like osteoarthritis, rheumatoid arthritis, avascular necrosis, certain fractures etc. Modern hip replacements make use of materials like titanium, ceramics, and cobalt-chrome that make them tough and durable. Age is not generally a concern when considering someone for a hip replacement as long as they have the right indication. Ten year survivorship in general is more than 95% for most established prostheses.
REVISION TOTAL HIP REPLACEMENT (FOR PREVIOUSLY FAILED HIP JOINT SURGERY)
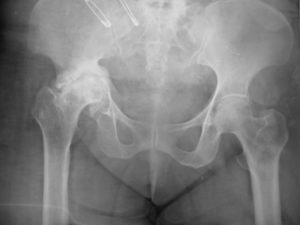
Primary hip and knee replacements do fail in for a number of reasons. Regular follow-up is essential for people with primary joint replacements. Revising them is highly specialised surgery requiring extensive training and access to sophisticated implants and hospital facilities. The old implant removed and replaced with new. Surgery may involve use of bone graft and/or custom made implants. Identifying failing joint replacements early is crucial for a successful outcome and therefore a regular follow-up by an orthopaedic surgeon is advised.
PRE-OPERATIVE PREPARATION
Patients have to undergo a full medical assessment prior to surgery. This includes and complete physical and psychological examination, x-rays and blood investigations, cardiology, physician and anaesthetic assessment.
Patients are also encouraged to engage with the physiotherapists to understand the exercises involved after surgery and the precautions they should take after surgery.
Conditions like diabetes and blood pressure should be well controlled prior to the surgery.
POST OPERATIVE INFORMATION
Following hip replacement surgery, patients usually remain in the hospital for 3 to 7 days. The length of recovery depends on the type of surgery performed (e.g., traditional, minimally invasive), the patient’s overall health, and the success of rehabilitation. After the procedure, patients must limit movement and the hip usually is braced in the correct position. Patients usually are required to do simple breathing or coughing exercises to reduce the risk for fluid in the lungs. Physical therapy often begins the day after surgery. Within 2 days, most patients are able to sit up, stand, and walk with assistance.